Understanding Sensory Processing in Children
You’ve probably been told your child is “too sensitive” or “not sensitive enough.” That they’re dramatic, or that they just need to get used to things. But what if their nervous system is simply processing the world differently and that difference has a name?
Sensory processing is one of the most talked-about, and most misunderstood, parts of neurodivergent development. This guide explains what it actually means, why it shows up the way it does, and what parents can do with that understanding.
What Is Sensory Processing?
Every second, your child’s nervous system is receiving an enormous amount of information from the world around them: sounds, textures, light, movement, temperature, the feeling of their own body in space. Sensory processing is the brain’s job of taking all of that input and deciding what to pay attention to, what to ignore, and how to respond.
For most people, this happens automatically and without much effort. For some children, particularly those who are autistic, have ADHD, or are otherwise neurodivergent, this process works differently. The brain may amplify certain signals, underrespond to others, or struggle to filter and organise the constant stream of input. The result is a child whose experience of the world is genuinely, neurologically different from what most adults assume.
The nervous system’s ability to adapt and reorganise -> a process called neuroplasticity -> plays a central role in how children develop sensory regulation over time.
This isn’t a behaviour problem. It’s a processing difference.
IMPORTANT NOTE
Sensory differences are not the result of bad parenting, lack of discipline, or a child being “difficult.” They reflect how a child’s nervous system is wired, and understanding that changes everything about how you support them.
More Than Five Senses
Most of us grew up learning about five senses. When it comes to sensory processing and neurodivergent children, there are actually eight worth knowing, and the three that often get overlooked are frequently the most significant.
TACTICLE
Touch
Sensory differences are not the result of bad parenting, lack of discipline, or a child being “difficult.” They reflect how a child’s nervous system is wired, and understanding that changes everything about how you support them.
AUDITORY
Sound
Volume, pitch, background noise. Some children hear things others barely notice, and it can be genuinely overwhelming.
VISUAL
Sight
Smell
The last three — vestibular, proprioceptive, and interoceptive — are the ones most relevant to behaviour, regulation, and emotional outbursts. They’re also the ones most often missed when a child is assessed for behavioural concerns alone.
Oversensitivity vs. Undersensitivity: Why Both Matter
Sensory differences don’t always look the same. A child can be oversensitive (hypersensitive) to some inputs and undersensitive (hyposensitive) to others, and many neurodivergent children experience both, in different sensory channels, at the same time.
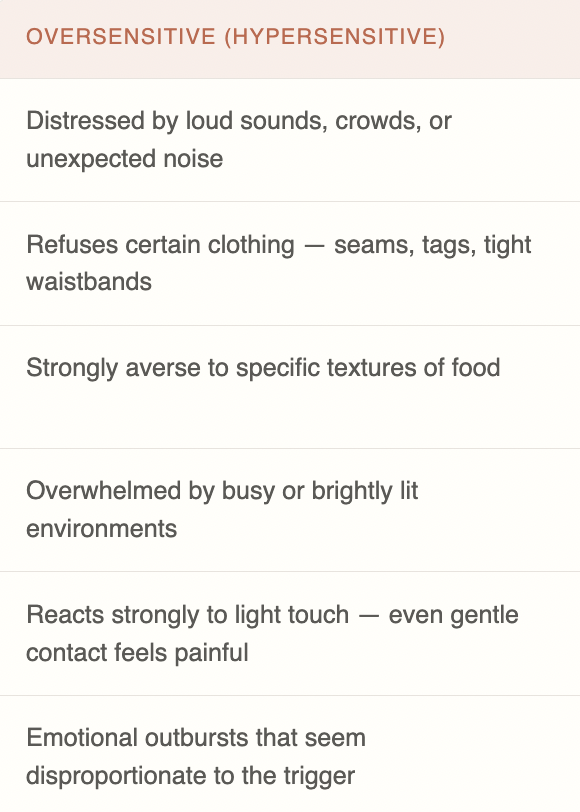

WORTH KNOWING
The same child can be hypersensitive to sound but hyposensitive to pain. Sensory profiles are individual, which is why a one-size-fits-all approach to support rarely works, and why understanding your specific child’s pattern matters so much.
How Sensory Differences Show Up Day to Day
In practice, sensory processing differences often don’t look like what parents expect. They show up as behaviour meltdowns, refusals, shutdowns, constant movement, rigid food preferences, difficulty with transitions, and they’re frequently misread as defiance, anxiety, or attention-seeking.
Some common examples parents often recognise once they understand what they’re seeing:
- Meltdowns or shutdowns in busy, noisy, or crowded places (supermarkets, birthday parties, school assemblies)
- Extreme distress about clothing: refusing to wear certain fabrics, socks, or shoes
- Very limited food repertoire based on texture, temperature, or appearance rather than taste alone
- Constantly seeking movement: spinning, jumping, climbing, especially indoors
- Covering ears, closing eyes, or hiding when overwhelmed
- Difficulty calming down after transitions or unexpected changes
- Bumping into things, difficulty with coordination, or seeming unaware of personal space
- Emotional outbursts that seem to come out of nowhere, but often follow sensory build-up
That last point is worth pausing on. Many emotional outbursts in neurodivergent children aren’t primarily emotional in origin, they’re the result of a nervous system that has been managing sensory overload all day and finally reached its limit. Understanding that changes how you respond to it.
Sensory Processing and the Nervous System
Sensory processing is fundamentally a nervous system function. The brain and body are in constant communication: receiving, filtering, interpreting, and responding to sensory input. When that communication is dysregulated, the effects are felt everywhere: in behaviour, attention, emotional regulation, sleep, digestion, and social connection.
This is why sensory differences rarely exist in isolation. In autistic children and those with ADHD, sensory processing differences often sit alongside challenges with attention, communication, and emotional regulation — not because they’re separate issues, but because they share the same underlying nervous system foundation.
Supporting the nervous system, helping it feel safer, more regulated, and better able to process incoming information, is increasingly understood as central to supporting neurodivergent children in all of these areas.
What Helps and What Doesn't
Once parents understand their child’s sensory profile, the instinct is to start removing triggers. That’s a good start, but it’s only part of the picture.
What tends to help: Predictable routines that reduce the number of unexpected sensory surprises. Sensory breaks built into the day: quiet spaces, movement opportunities, access to preferred textures or inputs. Gradual, supported exposure to challenging sensory environments rather than forced immersion. And perhaps most importantly – being taken seriously, so the child doesn’t have to manage their sensory experience alone.
What tends not to help: Repeated forced exposure without support (“they just need to get used to it”). Punishing meltdowns that are, at their root, nervous system responses rather than choices. Treating the behaviour without understanding the sensory cause underneath it.
Accommodating your child’s sensory needs is not the same as giving in or avoiding all challenge. It’s about building a foundation of safety and trust from which your child can gradually expand their tolerance on their own timeline, with support, not through endurance.
The Role of Complementary Support
Many families find that conventional approaches — occupational therapy, sensory integration therapy — are enormously helpful, and they remain the recommended first line of support for sensory processing difficulties. Some families also explore additional approaches, particularly when regulation, nervous system support, or overall responsiveness to therapy feels stuck or inconsistent.
Understanding your child’s full picture — sensory, neurological, regulatory — gives any support approach a better starting point. The more accurately a family can describe what they’re seeing, the more tailored and effective the support can be.
When to Seek a Sensory Assessment
If what you’re reading here resonates — if you’ve been wondering whether your child’s reactions are “normal,” or if you’ve been told they’re just being difficult when something clearly feels genuinely distressing to them — a sensory or occupational therapy assessment is a reasonable next step.
An occupational therapist with sensory integration training can map your child’s specific sensory profile and recommend targeted strategies. If you suspect autism or ADHD is also part of the picture, a developmental assessment alongside is worth requesting.
You don’t need a diagnosis to start learning. Understanding what your child’s nervous system needs is valuable regardless of what label, if any, comes later.
→ Neurodivergent & neurodevelopmental support in Ottawa
Does it sound like your child?
At Sunrise Neuro Acupuncture Integrative Clinic, we work with families navigating early developmental concerns. Book a free 15-minute phone consultation to talk through what you’re seeing.
💡 Remember
Recovery is not a straight line. There will be good days and challenging days. What matters is consistent effort, appropriate support, and the courage to explore treatments that might help you reach your fullest potential. Neuroacupuncture is one more tool in your recovery toolkit—a tool backed by thousands of years of clinical experience and increasingly by modern research.
This article is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read in this article.
Sources & references
1. Foundational theory — Sensory Integration Ayres, A.J. (1972). Sensory Integration and Learning Disorders. Western Psychological Services. — The original framework the entire field is built on, developed by occupational therapist and neuropsychologist Dr. A. Jean Ayres at the University of Southern California.
2. Clinical research — Neural foundations of sensory integration Lane, S.J. et al. (2019). Neural Foundations of Ayres Sensory Integration®. Brain Sciences, 9(7). Published on PubMed/NIH. → pmc.ncbi.nlm.nih.gov/articles/PMC6680650
3. Sensory processing in autism — peer-reviewed research Kilroy, E., Aziz-Zadeh, L., & Cermak, S. (2019). Ayres Theories of Autism and Sensory Integration Revisited. Brain Sciences, 9(3). Published on PubMed/NIH. → pmc.ncbi.nlm.nih.gov/articles/PMC6468444
4. DSM-5 diagnostic criteria — sensory processing as a formal criterion for autism American Psychiatric Association (2013, revised 2022). Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5-TR). — Hyper/hyporeactivity to sensory input is formally listed under ASD diagnostic criteria (Criterion B4). Plain-language summary: autismspeaks.org/autism-diagnostic-criteria-dsm-5
5. STAR Institute for Sensory Processing — parent and clinical resource The leading research and education centre for sensory processing disorder globally. → sensoryhealth.org
6. Ayres Sensory Integration — University of Southern California USC Chan Division of Occupational Science, where sensory integration theory was originally developed and continues to be researched. → chan.usc.edu/about-us/sensory-integration
7. Sensory Integration — clinical overview (StatPearls / NCBI) Peer-reviewed clinical summary of sensory integration theory and practice. → ncbi.nlm.nih.gov/books/NBK559155
Table of Contents

About Denis Grounin →
Denis Grounin, former ER nurse practitioner, R.TCMP, R.Ac, is the Founder of Sunrise Neuro Acupuncture Integrative Clinic in Ottawa with over 30 years of acupuncture experience and neurological training since the 1990s. His work focuses on neuro-acupuncture, rehabilitation support, and integrative neurological care.
Learn more about integrative medicine
Looking for a treatment?
Experience the benefits of Traditional Chinese Medicine with personalized care for your health.
